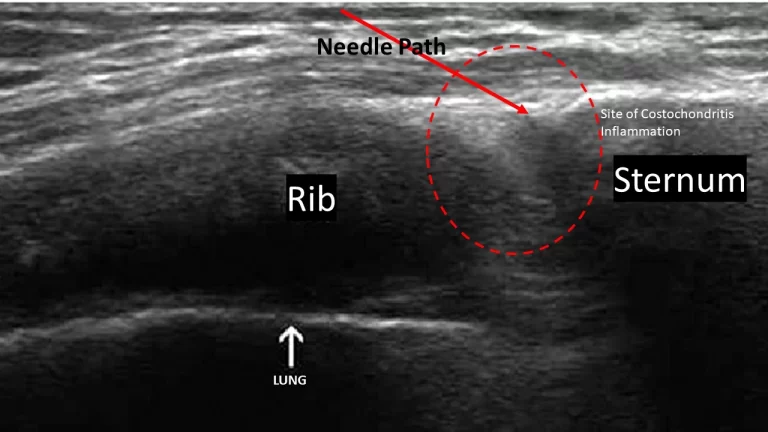
Costochondritis
Costochondritis, an inflammation of costochondral junctions of ribs or chondrosternal joints of the anterior chest wall, is a common condition seen in patients presenting to the physician’s office and emergency department. Palpation of the affected chondrosternal joints of the chest wall elicits tenderness. Although costochondritis is usually self-limited and benign, it should be distinguished from other, more serious causes of chest pain. Coronary artery disease is present in 3 to 6 percent of adult patients with chest pain and chest wall tenderness to palpation. History and physical examination of the chest that document reproducible pain by palpation over the costal cartilage is usually all that is needed to make the diagnosis in children, adolescents, and young adults. Patients older than 35 years, those with a history or risk of coronary artery disease, and any patient with cardiopulmonary symptoms should have an electrocardiograph and possibly a chest radiograph. Consider further testing to rule out cardiac causes if clinically indicated by age or cardiac risk status.