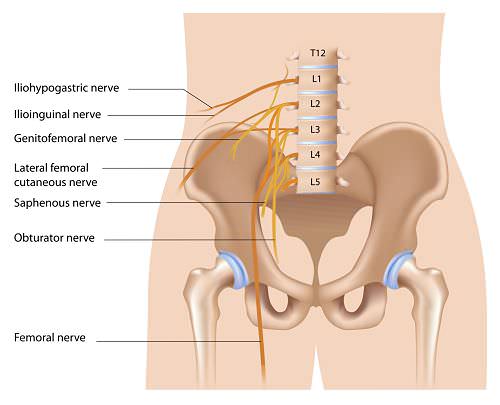
Compression injury to the lumbosacral plexus during labor and delivery, known as postpartum lumbosacral plexopathy, is underappreciated and often misdiagnosed. Although most large series place the incidence of this disorder at one in 2600 births, there are likely many milder cases that never reach medical attention.
The mechanism of injury likely involves compression of the fetal head against the underlying pelvis and lumbosacral plexus. Postpartum lumbosacral plexopathy results primarily from compression of the lumbosacral trunk. These are the fibers from the L4 and L5 roots, which join together to descend into the pelvis to reach the sacral plexus. When the lumbosacral trunk crosses the pelvic outlet, the fibers lie exposed (no longer protected by the psoas muscle) as they rest against the sacral ala near the sacroiliac joints. At this point, the fibers are most exposed and susceptible to compression. The origin of the superior gluteal nerve lies close by and may also be compressed. The fibers that eventually form the peroneal division of the sciatic nerve lie posteriorly, closest to the bone, and are more vulnerable to compression than the tibial division fibers. Accordingly, peroneal fibers are often most affected, with some women presenting with a postpartum footdrop, not infrequently misdiagnosed as peroneal palsy at the fibular neck.
Weakness may be noticed immediately or within the first few days after delivery. In addition to peroneal weakness, examination often shows mild weakness of knee flexion (hamstrings) and hip abduction, extension, and internal rotation (glutei, tensor fascia latae), demonstrating that the lesion is clearly beyond the peroneal territory. Sensory disturbance is most marked over the dorsum of the foot and lateral calf but may be patchy and involve the sole of the foot, posterior calf, and thigh.
Several factors predispose to this injury, including a first pregnancy, a large fetal head with a small maternal pelvis (cephalopelvic disproportion), a small mother (less than 5 feet in height), and a prolonged or difficult labor. Although rare patients may be left with permanent weakness, the prognosis is excellent in most cases. The presumed mechanism of injury involves compression that leads to ischemia and mechanical deformation of nerve fibers, which in turn lead to demyelination and, if severe enough, axonal loss. There is no tearing, shearing, or disruption of basement membranes. Thus, even in cases with severe axonal loss, recovery often is complete.