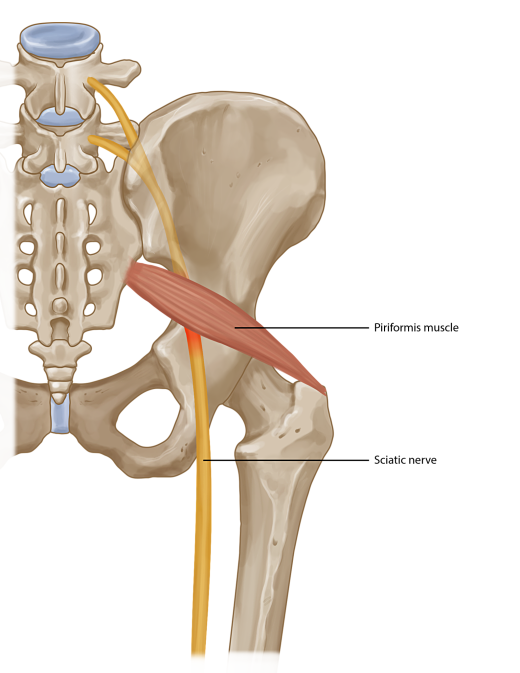
Luckily, there are some simple things you can do to prevent and ease (albeit not cure) piriformis syndrome:
Stretch, stretch, stretch: You guys—stop skipping your post-run stretch. It’s one of the five things all physical therapists desperately want runners to do to avoid injury. Your two best bets for stretching out that piriformis? Figure four stretch and pigeon pose, says Yellin. Do three to five repetitions, holding for 30 seconds each. (While you’re at it, add these 11 yoga poses perfect for runners to your routine.)
Soft tissue work: “Imagine getting a knot in your shoelace,” says Yellin. “What happens when you pull the string? It gets tighter. Sometimes just stretching isn’t enough, and you have to actually target specific spots.” The fix? Try self-myofascial release (with a foam roller or a lacrosse ball) or a see a massage therapist for active release. (Just don’t foam roll your IT band.)
Address your muscle imbalances. Many weekend warriors (people with desk jobs who are active outside the office) have tight hip flexors from sitting all day, says Yellin, which can mean they also have weak glutes as a result. You can pinpoint this and other muscle imbalances by seeing a physical therapist. (You can DIY it a little at home with these five steps to nix muscle imbalances, but a professional can give you the full workup.)
Just remember that these aren’t a permanent solution: “It’s just like anything with strength and flexibility: You put all that work in to make the gains,” says Yellin. If you stop doing the stretches or strengthening exercises that helped eliminate your piriformis syndrome, there’s a high likelihood of it returning, he says.
For more exercises for managemnt of Piriformis Syndrome, please click the link below:
https://www.painspa.co.uk/exerises-for-piriformis-pain/