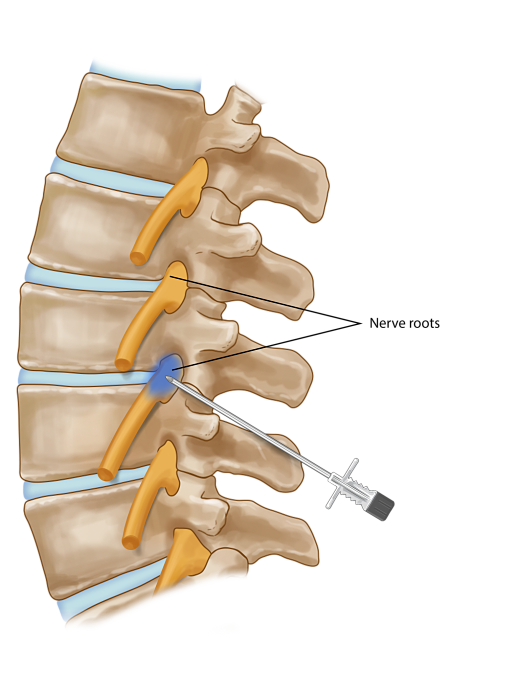
Nerve Root Block Summary
Nerve root block can provide pain relief in patients experiencing pain in the upper or lower limbs and in the thoracic area secondary to nerve root irritation at the spinal level. Nerve root blocks can also provide important diagnostic information that may formulate further management plan. However it is important to note that in some cases injection treatment may not provide the desired results or the pain relief may not be sustained. At Pain Spa Dr. Krishna always performs nerve root blocks under real time fluoroscopy guidance, using state of the art equipment. This ensures 100% accuracy and our complication rates are extremely low.
At Pain Spa we offer cervical, thoracic and lumbar nerve root blocks under fluoroscopy guidance. Dr Krishna is very experienced in these procedures and has a very meticulous approach and safety record.
Information Sheet