About Pain Spa
We focus on a holistic approach to pain management, encouraging healthy life style changes and promoting overall well-being.
Find out more
About Pain Spa
We focus on a holistic approach to pain management, encouraging healthy life style changes and promoting overall well-being.
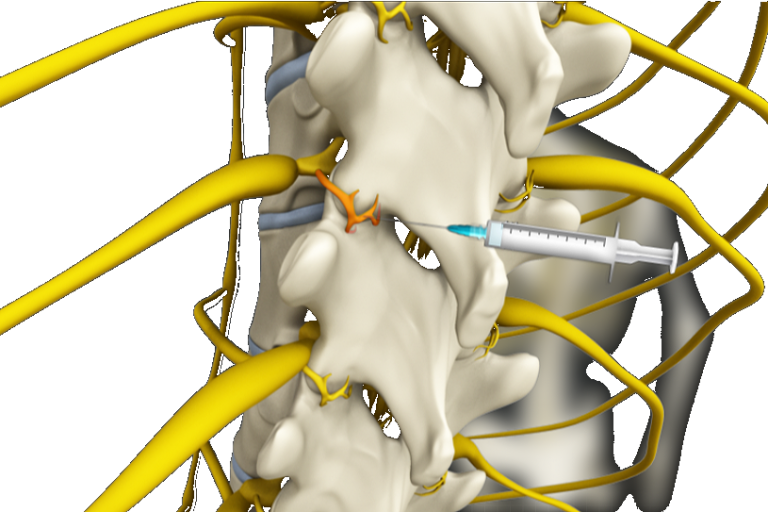
 Radiofrequency neurotomy is recognised as an effective minimally invasive treatment for chronic pain originating in the facet joints. But in order to deliver relief for patients suffering from debilitating pain, successful RF lesioning requires reaching the pain source. Until now, a major challenge in effectively treating chronic thoracic facet pain has been the variable course of the medial branch nerve, particularly at levels T5 to T8.
Radiofrequency neurotomy is recognised as an effective minimally invasive treatment for chronic pain originating in the facet joints. But in order to deliver relief for patients suffering from debilitating pain, successful RF lesioning requires reaching the pain source. Until now, a major challenge in effectively treating chronic thoracic facet pain has been the variable course of the medial branch nerve, particularly at levels T5 to T8.