ME/ CFS is a real illness, genetic study shows

By Sarah Knapton, Science Editor, Published in The Telegraph, 06 Aug 2025
A genetic cause for ME has been found for the first time, proving the illness is real.
In a breakthrough that charities said finally provided “credibility and validity” for sufferers, the University of Edinburgh found eight areas of genetic code that make a diagnosis more likely.
The gene activity was seen mainly in the nervous and immune systems, suggesting that people with ME may struggle to clear infections and experience ongoing symptoms of pain, fatigue and illness that other people recover from.
Sonya Chowdhury, co-investigator on the study and chief executive of Action for ME, said: “For years, many people have been maligned and disbelieved, and our findings will change this.
“We know that many people have experienced comments like ‘ME’s not real’. They’ve been to doctors and told that it’s not a real illness.
“Being able to take this study into the treatment room and to say there are genetic causes that play a part in ME is going to be really significant. It will rebuff that lack of belief and stigma that exists.”
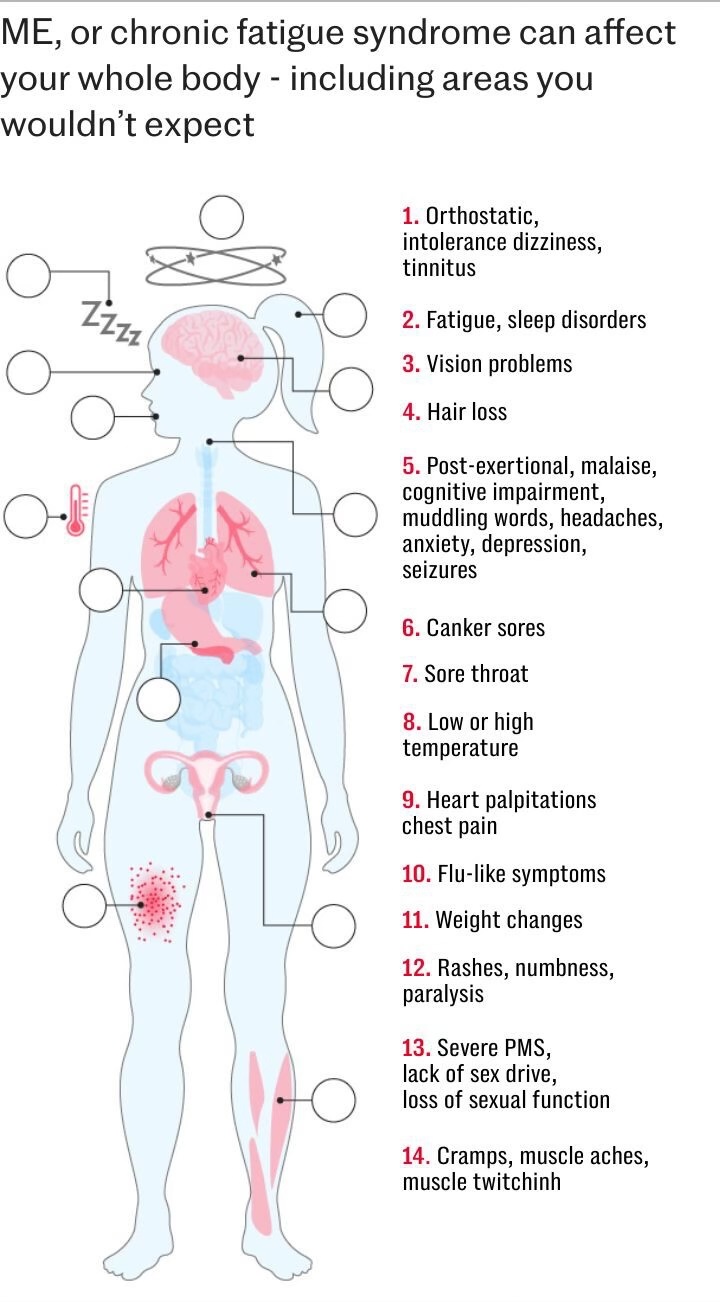
ME, or myalgic encephalomyelitis – which is often known as chronic fatigue syndrome – is a long-term illness characterised by extreme fatigue that is not relieved by rest, and may bring malaise after exercise, sleep problems, brain fog and chronic pain.
About 1.35 million people in Britain are thought to suffer with some kind of ME-like symptoms, which often occur following an infection such as flu, Covid or Epstein-Barr.
But the vagueness of the illness and difficulty finding a trigger has often led patients to be treated with scepticism, even by medical professionals. In the past, the condition was regularly dismissed as “yuppie flu”.
For the new study, researchers analysed the DNA of more than 15,000 people participating in DecodeMe – the world’s largest database of people with the disease.
They found eight regions of DNA where genetic differences were significantly more common in people with ME/chronic fatigue syndrome than in the general population.
As a person’s DNA does not change over time, experts say the genetic signals likely reflect the causes of the disease.
Prof Chris Ponting, DecodeME investigator from the University of Edinburgh, said: “What we are looking at is genetic variants which tilt the balance one way or another towards or away from the risk of diagnosis of ME in exactly the same way as (genes) do for diabetes or Parkinson’s.
“These genetic signals lie very close to genes which are now well known to be involved in the first response to infection, and so it could very well be for some people that an infection via viruses or bacteria are less well cleared with people with ME.
“People with ME often report an infection before their first onset of symptoms. This occurs with the majority of people with ME, so overall the genetics align with what people have described.”
Among the genes involved is RABGAP1L, which limits virus replication and expels bacteria, but is less active in patients with ME.
Another is FBXL4, which is crucial for keeping mitochondria – the cell batteries – functioning correctly, but is under-expressed in some people with ME.
How to treat chronic fatigue syndrome – the conventional view
There is currently no conventional cure for CFS, which is also known as ME.
However, according to the NHS, Most people with CFS will improve over time, especially with treatment, although some people do not make a full recovery, the following approaches might work:
- Cognitive behavioural therapy, if anxiety presents as part of the problem
- Energy management – where the patient is given advice about how to make best use of the energy they have without making their symptoms worse
- Medication to control symptoms such as pain and sleeping or mood issues
Researchers say the findings are not yet ready to inform treatment or diagnosis, but offer vital clues to the disease’s origins and could guide future drug development.
Andy Devereux-Cooke, an ME patient who has worked as a co-investigator on the project, said the findings were important for patients who had felt “abandoned”.
“This will be huge for the patient population,” he said.
“Even though it does not provide all the answers, it is a welcome drop in the ocean towards turning the tide.”
The DecodeME team is now calling on researchers from around the world to use the dataset to develop new studies that could lead to new insights and possible treatments.